JBRA Assist. Reprod. 2019;23(4):328-332
ORIGINAL ARTICLE
doi: 10.5935/1518-0557.20190014
Intrauterine insemination as a primary viable option to infertile couples: evaluation of patients in a private center
1Gynecology and Obstetrics Post Graduation Program of Federal University of Paraná (UFPR) PR - Brazil
2Positivo University (UP). Curitiba - PR - Brazil
3Conceber Reproductive Medicine Center. Curitiba - PR - Brazil
4Department of Obstetrics and Gynaecology of Federal University of Paraná (UFPR) - Curitiba - PR- Brazil
CONFLICT OF INTEREST
The authors have no conflicts of interest to declare.
ABSTRACT
Objective: This study aimed to identify which parameters positively affect the clinical pregnancy rates of IUI cycles and find which couples should opt for IUI.
Methods: This retrospective observational study included 261 patients submitted to 381 IUI cycles with fresh or cryopreserved partner semen (IU-H) from January 2012 to February 2017 in a private center in Curitiba-PR, Brazil.
Results: Idiopathic infertility was the most frequent finding (35.9%). Patients younger than 40 years accounted for 87.9% of the IUI cycles (n=335) and 16.1% of the clinical pregnancies (n=54). The pregnancy rate was three times higher in patients with an endometrium thickness ≥8 mm compared to patients with endometrium thickness <8mm. Sperm motility >55% was linked to higher pregnancy rates (p=0.002). Concerning gonadotropins, 159 (48.4%) took rFSH, 127 (38.7%) hMG, and 42 (12.8%) uFSH, with pregnancy rates of 21.3%, 10.4% and 10.5%, respectively.
Conclusion: Patients under 40 years of age with endometrium thickness ≥8 mm, sperm motility >55%, and on rFSH had significantly higher pregnancy rates (p<0.05).
Keywords: Intrauterine insemination, endometrial thickness, recombinant follicle stimulating hormone, sperm motility.
INTRODUCTION
The demand for infertility treatment has grown exponentially in Brazil. Intrauterine insemination (IUI) is a low complexity fertility treatment that is much less invasive and inexpensive when compared to in vitro fertilization (IVF) (Isa et al., 2014a). Pregnancy rates after IUI vary widely due to multiple patient-related factors (Isa et al., 2014a; 2014b; Allen et al., 1985; Asante et al., 2013; Nuojua-Huttunen et al., 1999; Schuffner et al., 2009). IUI can be indicated for patients with different causes of infertility, including cervical factor infertility, ovulatory dysfunction, endometriosis, infertility for immunological causes, and idiopathic infertility (Duran et al., 2003).
Some factors may have a decisive role in the outcome of IUI, such as age, ovarian reserve, endometrial thickness, types and doses of gonadotropin, and sperm quality. Although several studies have searched for markers of success in IUI, age remains as the best parameter to assess ovarian function and consequently the response to assisted reproductive technologies (Deatsman et al., 2016). Although some authors have linked higher levels of AMH to higher pregnancy rates (Bakas et al., 2015), the predictive value of AMH remains questionable in scientific literature (Tremellen & Kolo, 2010).
Endometrial thickness has been associated with higher embryo implantation and IUI success rates. There is no consensus in the literature over an ideal cutoff value, although most studies agree on endometrial thickness greater than 7 mm (Biswas et al., 2016; Caetano et al., 2005).
IUI without controlled ovarian stimulation is not recommended, as natural cycles offer no clinical advantage. Fertility rates are higher in stimulated cycles (Rashidi et al., 2013; Fritz & Speroff, 2011). In several countries, it is mandatory to register IUI procedures. In Denmark, for example, IUI treatments have been registered since 2007 (Malchau et al., 2014). REDLARA, the Latin American Network of Assisted Reproduction, reported 6,250 cycles of IUI in 2013 with a birth rate per cycle of 14.9% (Zegers-Hochschild et al., 2016). In Brazil, outcomes and indications of IUI are scarce.
The aim of the study was to identify which parameters positively affected the clinical pregnancy rates of IUI cycles in a private assisted reproduction center and evaluate which couples should opt for IUI.
MATERIAL AND METHODS
Patients
This retrospective observational study included 261 patients submitted to 381 IUI cycles with fresh or cryopreserved partner semen (IU-H) from January 2012 to February 2017 in a private center in Curitiba-PR, Brazil. Heterologous intrauterine insemination procedures were not included, so as not to affect pregnancy rates.
The local institutional review board approved the study. Patients were not required to give consent due to the retrospective nature of the study.
The included subjects were split into groups based on the cause of infertility, age, endometrial thickness (measured two days before IUI), and anti-Müllerian hormone (AMH) levels. AMH levels were measured in 125 patients, and test results were not considered for IUI. The groups were further divided between fresh vs. frozen semen and levels of sperm concentration and motility.
Controlled ovarian stimulation
Controlled ovarian stimulation was achieved by three different protocols: 1) Injectables, 2) Oral medication + injectables, 3) Oral medication. Group 1 was divided into three subgroups: A) human menopausal gonadotropin (hMG) - Menopur®, B) recombinant follicle stimulating hormone (rFSH) - Gonal® or Pergoveris®, and C) urinary follicle stimulating hormone (uFSH) Fostimon®. Group 2 took clomiphene citrate (CC) followed by the injectable medications cited above. Group 3 took CC or Letrozole®. The final outcome considered for all variables was clinical pregnancy.
Serial transvaginal ultrasound examination was performed on the second or third day of the cycle and on the sixth day after the start of controlled ovarian stimulation. The remaining tests varied according to the response each patient had to the stimulation protocol. hCG (Choriomon® or Ovidrel®) was administered when the mean diameter of the dominant follicle reached at least 18mm. IUI was scheduled 36h to 40h thereafter. Endometrial thickness was evaluated 48h before IUI, without later analysis. Supplementation of the luteal phase with Utrogestan® or Duphaston® was also performed.
Semen Processing
Semen samples were processed by density gradient centrifugation or sperm wash according to the 2010 guidelines of the World Health Organization (WHO) for semen processing (WHO, 2010). Sperm wash was performed in samples meeting the following criteria: increased viscosity, concentration <15 million per ml, and motility <32%. Other samples underwent density gradient centrifugation. In both procedures, the volume was measured after collection and concentration and motility were evaluated on Makler chambers with the aid of a light microscope.
After complete liquefaction in density gradient centrifugation, the semen samples were processed with density gradient medium (Isolate, Irvine Scientific, California) and sperm washing medium (Modified HTF Medium HEPES with Gentamicin, Irvine Scientific, California). In the processing technique, 90% and 45% colloidal gradient were used. One mL of the lower phase gradient was transferred into a sterile disposable conical-bottom centrifuge tube using a Pasteur pipette. A second 1 mL layer of the upper phase was gently placed on top of the lower phase. Liquefied semen was gently placed onto the upper phase. The sample was centrifuged for 20 minutes at 516G. The supernatant was discarded, and the pellet was resuspended with a Pasteur pipette in 2.5 mL of HTF. Sperm wash was performed with centrifugation for eight minutes at 516G. Then the supernatant was discarded and the pellet resuspended with a Pasteur pipette in 0.5 mL of HTF. Sperm parameters were then evaluated according to the WHO criteria for IUI.
Statistical analysis
Data were organized on Microsoft Office Excel 2007® and analyzed on SPSS Statistics 22.0®. The results were expressed as frequencies and proportions for categorical and qualitative variables, and as measures of dispersion and central tendency for quantitative variables.
The Mann-Whitney test for quantitative variables was used to assess the relationship between clinical/biological variables and pregnancy success. The non-parametric Shapiro-Wilk test was chosen to test the normality of quantitative variables. The Chi-square or Fisher's exact test was used to test the association between qualitative variables and the outcome of treatment. Statistical significance was attributed to comparisons with a p-value <0.05.
Linear logistic regression models were used to determine the relationship between outcomes and the clinical/biological variables. Explanatory variables with a significance level of up to 20% in univariate analysis were included in the logistic regression model. The results were expressed as odds ratios (OR).
Statistical power analysis was performed to verify the ability of tests to reject a false null hypothesis. Software program GPower 3.1 was used in the analysis of statistical power from univariate and multivariate analysis.
RESULTS
Idiopathic infertility was identified in 35.9% of the cases, followed by ovulatory dysfunction with 26.2% and endometriosis with 15.2%. Other less frequent causes were cervical factor, tubal factor, male factor and multiple factor infertility. There was no statistical difference regarding the cause of infertility and the number of pregnancies (p=0.8). Fifty-six (14.6%) of the 381 cycles analyzed resulted in clinical pregnancy.
Patients younger than 40 years accounted for 87.9% (335) of the sample and achieved 54 clinical pregnancies (16.1%). The clinical pregnancy rate was five times higher in younger patients (<40 years) compared to their older peers (>40 years) (p=0.043). Among the patients with positive clinical pregnancies, only two were older than 40 years (Table 1). When the patients were split by age (≤29, 30-34, 35-39, and ≥40 years), most pregnancies - 26 (6.8%) - occurred between 35 and 39 years of age (Table 2), but the groups were not statistically different (p=0.156).
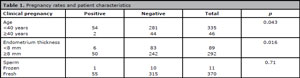
Table 1. Pregnancy rates and patient characteristics
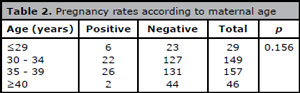
Table 2. Pregnancy rates according to maternal age
Endometrial thickness >8mm was found in 76.6% (292) of the patients. Patients with an endometrial thickness greater than 8 mm were three times more likely to achieve clinical pregnancies than the individuals with an endometrial thickness <8mm (p=0.016). Of the 89 patients with endometrial thickness <8mm, only six (6.7%) achieved clinical pregnancies (Table 1).
Fresh semen samples were more frequent (97.1%), and sperm concentration ranged from 2 to 300 million per mL, while sperm motility ranged from 8.1% to 95% after processing. Cryopreserved semen was used in 11 procedures, and only one patient achieved clinical pregnancy. Motility above 55% had higher rates of clinical pregnancy (p=0.002).
Of the 381 cycles analyzed, 328 (86.0%) were from Group 1 (injectables) (Table 3), and 42 (11.0%) were from Group 2 (injectables plus oral medication). Nine patients (2.3%) took only oral drugs and two (0.52%) did not use medication. The group given oral medication alone and the individuals undergoing medication-free natural cycles did not achieve clinical pregnancy.
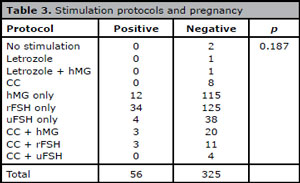
Table 3. Stimulation protocols and pregnancy
In the group taking only injectables, 159 patients (48.4%) took rFSH, 127 (38.7%) were on hMG, and 42 (12.8%) on uFSH, yielding clinical pregnancy rates of 21.3%, 10.4%, and 10.5%, respectively. Patients on rFSH achieved clinical pregnancy rates 2.5 times higher than the individuals on hMG (p=0.02) (Table 4). Six (14.2%) of the 42 patients in Group 2 achieved clinical pregnancies, three with clomiphene citrate and rFSH and three with clomiphene citrate and hMG.
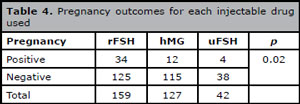
Table 4. Pregnancy outcomes for each injectable drug used
DISCUSSION
It is important to point out that even in patients diagnosed with idiopathic infertility, fertility rates may decline due to lower oocyte quality, fertilization failure or embryo implantation abnormalities (Wolff et al., 2013). Advanced maternal age is an established independent negative prognostic factor for live births and clinical pregnancy associated with lower chances of spontaneous or assisted pregnancy (Geisler et al., 2017). In the present study, a clear relationship was observed between lower clinical pregnancy rates and advanced maternal age. IUI procedures do not achieve high pregnancy rates in this group. In another similar study carried out in Brazil, advanced maternal age was the only variable significantly correlated with success rates of IUI (Sicchieri et al., 2018). Adequate endometrial thickness is widely considered a decisive factor in the outcomes of ART treatments (Wolff et al., 2013). The finding in our study that more than 93% of the patients with endometrium thickness >8 mm did not achieve pregnancy corroborates other studies. In a large study enrolling 2,929 patients submitted to IUI with idiopathic infertility factor, the results plateaued at an endometrial thickness of 10 mm . The literature is still controversial in relation to very thick endometria (>14mm), and some studies suggested that there might be less favorable endometrial characteristics in this group, as well as lower implantation rates (Dietterich et al., 2002; Weissman et al., 1999). Some studies suggested that the ultrasound aspect of the endometrium (echogenicity) might be linked to higher implantation rates. This was not analyzed in the present study (Alborzi et al., 2005).
The link between increased pregnancy rates and increased sperm motility is in agreement with the literature (Duran et al., 2003). Few studies have looked into the outcomes of IUI with frozen semen. Our study corroborated the literature, suggesting lower pregnancy rates when frozen semen samples were used in IUI (Dinelli et al., 2014). Since our study featured a limited number of patients using frozen semen, more studies are needed to determine whether IUI should be carried out with frozen semen. Since motility is very important to achieving successful outcomes, it has been suggested that the causes of low sperm motility after semen processing, such as varicocele, should be corrected prior to assisted reproduction procedures (Hendin et al., 2000).
Although only a few patients did not take injectables in our study, cycles stimulated with injectable or oral medications and injectables only have reportedly greater chances of success. In a study by Malchau et al. (2014), 76% of the children born after IUI resulted from controlled ovarian stimulation with CC, FSH or both (Rashidi et al., 2013).
A trend toward higher pregnancy rates was observed with rFSH (Demirol & Gurgan, 2007), but the cost-effectiveness of this drug compared to hMG is questionable, since rFSH is more expensive than hMG (Gerli et al., 2008). In addition to providing better ovarian response, cycles with rFSH reportedly yield better quality oocytes (Cheon et al., 2004). Our study showed better results in stimulated cycles using rFSH, but the medication is not affordable by the standards of most of our patients. Moreover, positive pregnancy outcomes may also be achieved through other stimulation protocols.
CONCLUSION
IUI is a viable procedure and a good option for the initial treatment of infertile couples, since high pregnancy rates may be achieved when patients are adequately selected.
In this study, IUI patients younger than 40 years with endometrial thickness greater than 8mm had higher clinical pregnancy rates. Endometrial thickness may be an important parameter to be assessed in future research. Sperm motility also had a significant impact on the success of IUI cycles. Further studies are needed to evaluate whether frozen sperm negatively affects pregnancy rates.
Our results suggest that rFSH produces better outcomes than hMG, but more prospective controlled studies are needed to confirm the efficiency of these drugs in IUI.
The decision to perform the most appropriate treatment for each patient should be a priority in ART centers. It is important to carry out studies in each service and compare the findings with data from the literature.
Allen NC, Herbert CM 3rd, Maxson WS, Rogers BJ, Diamond MP, Wentz AC. Intrauterine insemination: a critical review. Fertil Steril. 1985;44:569-80.
Medline Crossref
Asante A, Coddington CC, Schenck L, Stewart EA. Thin endometrial stripe does not affect likelihood of achieving pregnancy in clomiphene citrate/intrauterine insemination cycles. Fertil Steril. 2013;100:1610-4.e1.
Medline Crossref
Bakas P, Boutas I, Creatsa M, Vlahos N, Gregoriou O, Creatsas G, Hassiakos D. Can anti-Mullerian hormone (AMH) predict the outcome of intrauterine insemination with controlled ovarian stimulation? Gynecol Endocrinol. 2015;34:765-8.
Medline Crossref
Biswas JK, Bandhu HC, Singh H, Dey M. Relation of endometrial thickness and pregnancy rates in intrauterine insemination following ovulation induction. Int J Reprod Contracept Obstet Gynecol. 2016;5:110-5.
Crossref
Caetano JPJ, Cota AMM, Sousa EBA, Lamaita RM, Moraes LAM, Aguiar LPT, Marinho RM. Comparison between three protocols for ovulation Induction in cycles of intrauterine insemination and related endometrial thickness and pregnancy rate achieved in each protocol. Rev Bras Ginecol Obstet. 2005;27:7-11.
Crossref
Cheon KW, Byun HK, Yang KM, Song IO, Choi KH YK. Efficacy of recombinant human follicle-stimulating hormone in improving oocyte quality in assisted reproductive techniques. J Reprod Med. 2004;49:733-8.
Medline
Deatsman S, Vasilopoulos T, Rhoton-Vlasak A. Age and Fertility: A Study on Patient Awareness. JBRA Assist. Reprod. 2016;20:99-106.
Medline Crossref
Demirol A, Gurgan T. Comparison of different gonadotrophin preparations in intrauterine insemination cycles for the treatment of unexplained infertility: a prospective, randomized study. Hum Reprod. 2007;22:97-100.
Medline Crossref
Dietterich C, Check JH, Choe JK, Nazari A, Lurie D. Increased endometrial thickness on the day of human chorionic gonadotropin injection does not adversely affect pregnancy or implantation rates following in vitro fertilization-embryo transfer. Fertil Steril. 2002;77:781-6.
Medline Crossref
Dinelli L, Courbière B, Achard V, Jouve E, Deveze C, Gnisci A, Grillo JM, Paulmyer-Lacroix O. Prognosis factors of pregnancy after intrauterine insemination with the husband's sperm: conclusions of an analysis of 2,019 cycles. Fertil Steril. 2014;101:994-1000.
Medline Crossref
Duran HE, Morshedi M, Kruger T, Oehninger S. Intrauterine insemination: a systematic review on determinants of success. Hum Reprod Update. 2003;8:373-84.
Medline Crossref
Geisler ME, Ledwidge M, Bermingham M, McAuliffe M, McMenamin MB, Waterstone JJ. Intrauterine insemination-No more Mr. N.I.C.E. guy? Eur J Obstet Gynecol Reprod Biol. 2017;210:342-7.
Medline Crossref
Gerli S, Bini V, Di Renzo GC. Cost-effectiveness of recombinant follicle-stimulating hormone (FSH) versus human FSH in intrauterine insemination cycles: a statistical model-derived analysis. Gynecol Endocrinol. 2008;24:18-23.
Medline Crossref
Hendin BN, Falcone T, Hallak J, Nelson DR, Vemullapalli S, Goldberg J, Thomas AJ Jr, Agarwal A. The effect of patient and semen characteristics on live birth rates following intrauterine insemination: a retrospective study. J Assist Reprod Genet. 2000;17:245-52.
Medline Crossref
Isa AM, Abu-Rafea B, Alasiri SA, Al-Mutawa J, Binsaleh S, Al-Saif S, Al-Sager A. Accurate diagnosis as a prognostic factor in intrauterine insemination treatment of infertile Saudi patients. J Reprod Infertil. 2014a;15:184-9.
Medline
Isa AM, Abu-Rafea B, Alasiri SA, Binsaleh S, Ismail KH, Vilos GA. Age, Body mass index, and number of previous trials: are they prognosticators of intra-uterine-insemination for infertility treatment? Int J Fertil Steril. 2014b;8:255-60.
Medline
Malchau SS, Loft A, Henningsen AKA, Nyboe Andersen A, Pinborg A. Perinatal outcomes in 6,338 singletons born after intrauterine insemination in Denmark, 2007 to 2012: the influence of ovarian stimulation. Fertil Steril. 2014;102:1110-6.e2.
Medline Crossref
Nuojua-Huttunen S, Tomas C, Bloigu R, Tuomivaara L, Martikainen H. Intrauterine insemination treatment in subfertility: an analysis of factors affecting outcome. Hum Reprod. 1999;14:698-703.
Medline Crossref
Rashidi M, Aaleyasin A, Aghahosseini M, Loloi S, Kokab A, Najmi Z. Advantages of recombinant follicle-stimulating hormone over human menopausal gonadotropin for ovarian stimulation in intrauterine insemination: a randomized clinical trial in unexplained infertility. Eur J Obstet Gynecol. 2013;169:244-7.
Medline Crossref
Sicchieri F, Silva AB, Silva ACJSRE, Navarro PAAS, Ferriani RA, Reis RMD. Prognostic factors in intrauterine insemination cycles. JBRA Assist Reprod. 2018;22:2-7.
Medline Crossref
Tremellen K, Kolo M. Serum anti-Mullerian hormone is a useful measure of quantitative ovarian reserve but does not predict the chances of live-birth pregnancy. Aust New Zeal J Obstet Gynaecol. 2010;50:568-72.
Medline Crossref
Weissman A, Gotlieb L, Casper RF. The detrimental effect of increased endometrial thickness on implantation and pregnancy rates and outcome in an in vitro fertilization program. Fertil Steril. 1999;71:147-9.
Medline Crossref
Wolff EF, Vahidi N, Alford C, Richter K, Widra E. Influences on endometrial development during intrauterine insemination: clinical experience of 2,929 patients with unexplained infertility. Fertil Steril. 2013;100:194-9.e1.
Medline Crossref
Zegers-Hochschild F, Schwarze JE, Crosby JA, Musri C, Urbina MT; Latin American Network of Assisted Reproduction (REDLARA) . Assisted reproductive techniques in Latin America: The Latin American Registry, 2013. J Bras Reprod Assist. 2016;20:49-58.
Medline Crossref