JBRA Assisted Reproduction 2013; 17 (2):98-100
ORIGINAL ARTICLE
doi: 10.5935/1518-0557.20130014
Is reliable the new semen analysis of the WHO laboratory manual for the diagnosis of the male factor in an infertile population?
É confiável a nova avaliação seminal da OMS(2010) para o diagnóstico do fator masculino numa população infértil?
Asociados en Reproducción Humana, Bogotá, Colombia.
Accredited Redlara center
ABSTRACT
Objective: The aim of this study was to compare the results of the semen analysis data while applying the parameters set out in the previous standard and the last proposed, in order to assess the changes in the diagnosis in terms of normal or abnormal, as how this fact can affect treatment decisions.
Methods: 1184 semen analysis of patients undergoing examination at our institution were reviewed, between January 2010 and September 2012 and were classified as normal or abnormal according to WHO parameters of 1999 and 2010 to be then compared. Exams of patients over 50 years (39 cases) were excluded for having found in this group a significant increase of asthenozoospermia when compared to younger ages.
Results: In the 1145 semen analysis studied, the average age of the patients was 37.4 years, and no significant difference was found while analyzing the absolute seminal variables of volume, motility and sperm morphology in the different age groups. Semen parameters in the 1999 classification had 42% of the samples reported as normal and 58% abnormal, but when applying the new classification,73% of the samples would be normal and only 27% abnormal. Analyzing sperm motility, 83% of the males were reported as normal with the WHO 2010 compared to a 77% with the WHO 1999 classification. However, the sperm morphology according to the WHO 2010, shows 95% of men within normal limits, whereas with the previous classification, only 39% of them would be fertile.
Conclusion: Based in our data, the sperm analysis as a single tool in the diagnosis of male factor should be revaluated.
Keywords: Semen analysis, WHO, infertility
RESUMO
Objetivo: Este estudo visou comparar os resultados dos dados de análise de sêmen com os parâmetros indicados na norma anterior e na última proposta da OMS (2010), a fim de avaliar as alterações no diagnóstico em termos de normal ou anormal, e como este fato pode afetar as decisões de tratamento.
Métodos: 1184 análises do sêmen de pacientes submetidos ao exame em nossa instituição foram revistos, entre janeiro de 2010 e setembro de 2012 e foram classificados como normais ou anormais de acordo com parâmetros da OMS de 1999 e 2010, para então ser comparados. Exames de pacientes com mais de 50 anos (39 casos) foram excluídos por termos encontrado neste grupo um aumento significativo de astenozoospermia quando comparado com idades mais jovens.
Resultados: A idade média dos pacientes era de 37,4 anos, e nenhuma diferença significativa foi encontrada ao analisar as variáveis absolutas seminais de volume, motilidade e morfologia espermática nas diferentes faixas etárias. Parâmetros seminais na classificação 1999 tinham 42% das amostras relatadas como normais e 58% de anormais, mas quando se aplica a nova classificação, 73% das amostras seriam normais e apenas 27% anormais. A motilidade dos espermatozóides em 83% dos homens foi relatada como normal (WHO 2010) em comparação com 77% sob a classificação WHO, 1999. No entanto, a morfologia dos espermatozóides de acordo com a OMS, 2010, mostra 95% dos homens dentro dos limites normais, enquanto que com a classificação anterior, apenas 39% deles seriam férteis.
Conclusão: Com base nos nossos dados, a análise de esperma de uma única ferramenta para o diagnóstico de factor masculino deve ser reavaliada.
Palavras-chave: análise do sêmen, a OMS infertilidade,
INTRODUCTION
The male factor involves up to 40% of the causes of infertility in couples and the semen analysis remains the initial study for the diagnostic of the male, having a high sensitivity (89%) and low specificity, however there are difficulties in laboratories for its standardization making the results among them inconsistent.
Since 1980, the WHO has published issues of the “Manual for the Examination of Human Semen”, and the last was done in 2010.
The aim of this study was to compare the results of the semen analysis data while applying the parameters set out in the previous standard and the last proposed, in order to assess the changes in the diagnosis in terms of normal or abnormal, as how this fact can affect treatment decisions.
MATERIALS AND METHODS
1184 semen analysis of patients undergoing examination at our institution were reviewed, as part of the study of infertility between January 2010 and September 2012 and were classified as normal or abnormal according to WHO parameters of 1999 and 2010 to be then compared.
Examinations of patients over 50 years (39 cases) were excluded for having found in this group a significant increase of asthenozoospermia when compared with younger ages.
Results: In the 1145 semen analysis studied, the average age of the patients was 37.4 years, and no significant difference was found while analyzing the absolute seminal variables of volume, motility and sperm morphology in the different age groups.
When analyzing semen parameters with the 1999 classification,42% of the samples analyzed were reported as normal and 58% abnormal, but when applying the new classification ,73% of the samples would be normal and only 27% abnormal.
Analyzing sperm motility, 83% of the males were reported as normal with the WHO 2010 compared with a 77% with the WHO 1999 classification.
However taking the sperm morphology parameter, according the WHO 2010, 95% of men are within normal limits, whereas with the previous classification, only 39% of them would be fertile.
DISCUSSION
Approximately 40% of couples with infertility problems have an isolated male factor or associated with a female factor, therefore, it is evident that a suitable study, approach and infertility handling of this origin is critical while defining the need for assisted reproductive procedures.
The semen analysis, despite being known as a basic analysis, is the cornerstone in the study of man’s fertility potential. The seminal analysis has important limitations regarding epidemiological studies since it has an operator dependent high variability, and at times appears as an independent variable of the man’s fertile potential, without evaluating advanced and deep biological studies , that will allow a better diagnostic, besides, this fact is one of the reasons for which andrologists and specialists in this area have sought the develop of more strict criteria regarding sperm assessment, thus trying to limit the bias generated by these variables. (Björndahl et al, 2002).
Since 1980, the WHO has published issues of the “Manual for the Examination of Human Semen”, the new manual for the examination and processing of human semen (WHO 2010), aims to standardize these values globally in all laboratories and researchers in reproduction, this release presents the information of 4500 men from 8 countries on three continents. Changes regarding concentration and sperm motility are the most accepted in different fertility laboratories, the new classification in motility offers fewer confounding variables, being more quantitative, since only three groups are analyzed: Progressive (A), No progressive (B) and immotile sperms (C).
The parameter undergoing the most activity compared with the previous classification was the sperm morphology, being the most controversial, since its values dropped dramatically from 14% to 4%, which has been considered in several countries as very low regarding male fertility.
Clearly, a high percentage of abnormalities in the sperm morphology are associated with the presence of a poor sperm function, either in mobility or vitality, thus, finding a low percentage of normality as 4% in a semen sample, typically low levels of spermatozoa type A, B and vital are reported. (Cardona Maya, 2010).
The interest in morphology as a tool in the assessment of the man’s fertile potential was generated in 1900, when it became clear that normal and pathological forms can appear simultaneously in the same semen sample. (Agarwal & Said,2011) Since 1930 Moench and Holt reported that sperm morphology is the independent variable that can provide more information of the reproductive potential of the sperm. (1) Different authors have shown a negative correlation between the presence of large vacuoles in the nucleus of the sperm and the sperm chromatin stability, likewise it was observed that the increase of the fragmentation of the spermatic deoxyribonucleic acid (DNA) is associated to the presence of a greater number of abnormal forms.
The percentage of normal forms has been linked to exposure to toxic substances, chronic diseases and directly with the man’s fertility potential, therefore, while being altered, it will provide information that may be useful while preventing further systemic diseases .
The teratozoospermia has a deleterious effect on both the rate of fertilization and the pregnancy rate per IVF cycle, the latter secondary to the low rate of fertilization, but not to a poor embryo quality.
The low fertilization rate observed in patients with teratozoospermia is probably due to the affection in the binding and / or poor fusion of the oolema. Additionally pellucida zone is highly selective for normal spermatozoa, therefore the teratozoospermia has been correlated with decrease in the egg penetration by the sperm.
With the advent of in vitro fertilization, it has become clear that not all patients achieve fertilization despite having sperms in the ejaculation, however more recently, the development of the Intra-Cytoplasmic Sperm Insemination (ICSI) technique has identified, despite of having some sperm, when the overall sample is affected by a high rate of teratozoospermia, the fertilization rates decrease, therefore, the comprehensive assessment of semen parameters has a high predictive value in the outcome of reproductive technologies and is one of the main objectives for professionals of andrology laboratories.
Taking as independent variables each of the evaluated aspects in the sperm analysis, is clear the significative difference between the two classifications when the parameter is the sperm morphology assesment.
The main difference involve de average of normozoospermic males based in the two classifications. Using morphology as independent variable, with the new WHO 2010, 95% of men were classified as normal compared with a 39% when the previous classification was used.
CONCLUSION
In our study, the new parameters of the WHO semen analysis 2010 qualifies as normal up to 31% of the infertile male population previously considered abnormal, which may mislead the clinician delaying the treatment.
It seems important to note that the WHO recommendation in addition to modifying the parameters previously established, clarifies that these values are just a guide for laboratories to obtain their own standards according to their population and the interpretation must be done in conjunction with the clinical information, therefore we suggest to perform this study in specialized laboratories with well-established parameters.
Based in our data we conclude that the sperm analysis as a single tool in the diagnosis of male factor should be revaluated.
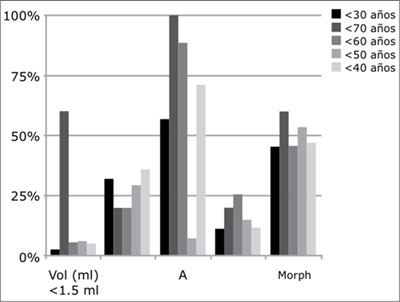
Figure 1. Difference in groups by age.
REFERENCES
Agarwal, A. & Said, T. Interpretation of basic semen analysis and advanced semen testing. In: Male Infertility: Problems and Solutions (Current Clinical Urology). 2011.pp. 15-22.
Crossref
Barratt, C.L.R., Naeeni, M., Clements, S. et al. (1995) Clinical value of sperm morphology for in-vivo fertility: comparison between World Health Organization criteria of 1987 and 1992. Hum. Reprod., 10, 587–593.
Medline
Björndahl L, Barratt CL, Fraser LR, Kvist U, Mortimer D. ESHRE basic semen analysis courses 1995–1999: immediate beneficial effects of standardized training. Hum Reprod 2002;17:1299-1305.
Medline Crossref
Cardona Maya, W. Manual de procesamiento de semen humano de la Organización Mundial de la Salud-2010. Actas Urol. Esp., 34(7):577-8, 2010.
Medline Crossref
Coetzee, K. . N. Bermes, W. Krause and R. Menkveld. Comparison of normal sperm morphology outcomes from two different computer-assisted semen analysis systems. Andrologia 33, 159-163 (2001)
Medline Crossref
Cohen-Bacrie P, Belloc S, Ménézo YJ, Clement P, Hamidi J, Benkhalifa M. Correlation between DNA damage and sperm parameters: a prospective study of 1,633 patients. Fertil Steril. 2009;91:1801-5.
Medline Crossref
Cooper TG, Noonan E, von Eckardstein S, Auger J, Baker HW, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update 2009 Nov 24. [Epub ahead of print].
Medline Crossref
Dorado Silva M, Migueles B, González M, Hebles M, Aguilera M, Sánchez P, et al. Relación entre los parámetros seminales y la fragmentación del ADN espermático. Rev Int Androl. 2008;6:14-7.
Crossref
Espinoza-Navarro, O. Sarabia. Evaluación y Estandarización de la Calidad del espermiograma: Nuevos Límites Inferiores de Referencia. Int. J. Morphol., 29(3):885-890, 2011.
Crossref
Grow DR, Oehninger S, Seltman HJ, Toner JP, Swanson RJ, Kruger TF, et al.: Sperm morphology as diagnosed by strict criteria: probing the impact of teratozoospermia on fertilization rate and pregnancy outcome in a large in vitro fertilization population. Fertil Steril. 1994; 62: 559-67.
Medline
Guzick DS, Overstreet JW, Factor-Litvak P, Brazil CK, Nakajima ST, et al. Sperm morphology, motility, and concentration in fertile and infertile men. N Engl J Med 2001; 345: 1388–93.
Medline Crossref
Jens Peter Ellekilde Bonde. Semen analysis from an epidemiologic perspective. Asian Journal of Andrology (2010) 12: 91–94.
Medline Crossref
Kruger TF, Menkveld R, Stander FS, Lombard CJ, Van der Merwe JP, van Zyl JA, et al.: Sperm morphologic features as a prognostic factor in in vitro fertilization. Fertil Steril. 1986; 46: 1118-23
Medline
Irvine DS, Twigg JP, Gordon EL, Fulton N, Milne PA, Aitken RJ. DNA integrity in human spermatozoa: relationships with semen quality. J Androl. 2000;21:33-44.
Medline
Irvine DS, Twigg J P, Gordon EL, Fulton N, Milne PA, Aitken RJ. DNA integrity in human spermatozoa: relationships with semen quality. J Androl. 2002;21:33-44.
Medline
Lamb, Dolores J.. Semen analysis in 21st century medicine: the need for sperm function testing. Asian Journal of Andrology (2010) 12: 64–70.
Medline Crossref
Menkveld R, Stander FS, Kotze TJ, Kruger TF, van Zyl JA. The evaluation of morphological characteristics of human spermatozoa according to stricter criteria. Human Reprod 1990; 5: 586–92.
Medline
Menkveld R, Wai Yee Wong, Carl, J Lombard, Alex M.M Wetzelds. Semen parameters, including WHO and strict criteria morphology, in a fertile and subfertile population: an effort towards standardization of in-vivo thersholds. Human Reproduction, 2001, vol 16, No. 6, pp. 1165-1171.
Medline Crossref
Menkveld R. Clinical significance of the low normal sperm morphology value as proposed in the fifth edition of the WHO Laboratory Manual for the Examination and Processing of Human Semen. Asian Journal of Andrology (2010) 12: 47–58.
Medline Crossref
Milton Ghirelli-Filho, Françoise Elia Mizrahi, Antonio Carlos Lima Pompeo, Sidney Glina. Influence of strict sperm morphology on the results of classic in vitro fertilization. Int Braz J Urol. 2012; 38: 519-28.
Medline Crossref
Mortimer D, Menkveld R. Sperm morphology assessment–historical perspectives and current opinions. J Androl 2001; 22: 192–205
Medline
Smith R, Kaune H, Parodi D, Madariaga M, Ríos R, Morales I, et al. Increased sperm DNA damage in patients with varicocele: relationship with seminal oxidative stress. Hum Reprod. 2006;21:986-93.
Medline Crossref
Wong, W,Y., Thomas, C.M.G., Merkus, J.M.W.M. et al. (2000) Male factor subfertility: possible causes and impact of nutritional factors. Fertil. Steril., 73, 435–442.
Medline Crossref
Zinaman MJ, Brown CC, Selevan SG, Clegg ED. Semen Quality and human fertility: a prospective study with health couples. J Androl 2000; 21: 145–53.
Medline